Hypersensitivity reactions: what they look like and what to do
Hypersensitivity reactions are when your immune system overreacts and harms you instead of helping. They range from a mild rash to life-threatening anaphylaxis. This page gives clear, practical steps for spotting, treating, and preventing these reactions so you can act fast and stay safer.
Types and how they show up
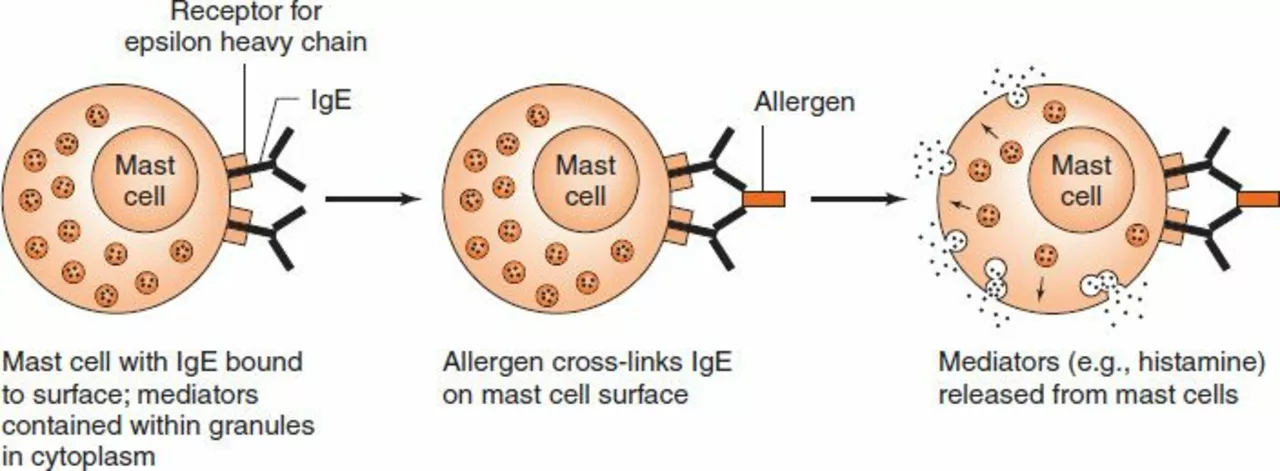
Doctors divide hypersensitivity into four main types. Type I is immediate and IgE‑mediated — think classic allergy: hives, sneezing, wheeze, throat tightness, or sudden low blood pressure after exposure to foods, insect stings, or some drugs. Type II involves antibodies attacking your own cells, which can cause anemia or kidney problems. Type III comes from immune complexes and shows as joint pain, fever, or skin rashes days after exposure. Type IV is delayed and cell‑mediated — contact dermatitis (from poison ivy or latex) and some drug rashes fit here and usually appear 48–72 hours later.
Recognize the timeline: immediate symptoms within minutes to hours suggest Type I; delayed symptoms days later point to Type III or IV. That helps when deciding how urgent care should be.
Quick steps during an allergic reaction
If someone has mild symptoms like localized hives or itching, remove the trigger if possible, give an oral antihistamine, and monitor. For breathing trouble, swelling of the face or throat, dizziness, or collapse — treat it as anaphylaxis: call emergency services and give intramuscular epinephrine right away if available. Lay the person flat with legs raised unless they vomit or can’t breathe. One dose of epinephrine can save a life; delay makes outcomes worse.
Mild skin rashes after a new drug still need assessment. Stop the medication and contact a healthcare provider. Severe skin reactions with blistering, mucosal sores, high fever, or widespread peeling (think Stevens‑Johnson syndrome or toxic epidermal necrolysis) require emergency care and hospitalization.
For suspected drug allergies, an allergist can do tests: skin testing for some antibiotics, blood tests for specific IgE, patch testing for contact allergies, or supervised drug challenge when safe. Never retry a drug linked to a severe reaction without specialist input.
Reducing future risk is practical: avoid known triggers, wear a medical ID if you have life‑threatening allergies, carry two epinephrine autoinjectors if prescribed, and tell all your healthcare providers about allergies. For some inhalant or venom allergies, immunotherapy (allergy shots or sublingual tablets) reduces reactions over time. For drug allergies, your doctor may suggest safer alternatives or desensitization in controlled settings.
Report serious adverse reactions to your doctor and local health authorities so other patients benefit. If you ever doubt how serious a reaction looks, seek emergency care — quick action saves lives.
How to manage abacavir hypersensitivity reactions
As a blogger who has researched abacavir hypersensitivity reactions, I've discovered some key steps to manage this condition. First, it's vital to get tested for the HLA-B*5701 allele, as it can help determine if you're at risk. If you experience symptoms like fever, rash, or gastrointestinal issues after starting abacavir, contact your healthcare provider immediately. They might recommend stopping the medication and not restarting it, as it could lead to severe complications. Lastly, always report any suspected reactions to your medical team to ensure proper care and management.
- May 29 2023
- Tony Newman
- 19 Comments
