Swallowing seems simple-until it doesn’t. If you’ve ever felt food stick in your chest, had trouble getting liquids down, or experienced chest pain that feels like a heart attack, you might be dealing with something more serious than indigestion. These symptoms often point to esophageal motility disorders, conditions where the muscles of the esophagus don’t work the way they should. Unlike GERD, where stomach acid backs up, these disorders are about movement-specifically, the failure of coordinated muscle contractions to push food into the stomach.
What Exactly Is Happening in the Esophagus?
Your esophagus isn’t just a passive tube. It’s a muscular pipeline that contracts in a wave-like motion called peristalsis. Think of it like squeezing a toothpaste tube from the bottom up-each contraction pushes food forward. In esophageal motility disorders, this wave breaks down. Sometimes it’s too weak. Sometimes it’s too strong. Sometimes it happens in the wrong order. The result? Food lingers, gets stuck, or even comes back up.The most common symptom is dysphagia-difficulty swallowing. It usually starts with solids, then progresses to liquids. People often describe it as food "sticking" or "pausing" behind the breastbone. Other signs include regurgitation of undigested food, chest pain, and unintentional weight loss. Surprisingly, many patients are misdiagnosed with acid reflux for years. They take proton pump inhibitors (PPIs) daily, but nothing changes because the problem isn’t acid-it’s muscle function.
How Do Doctors Know It’s Not Just GERD?
The first step is usually an upper endoscopy. A camera is passed down the throat to check for blockages, inflammation, or tumors. If nothing’s found, the next step is esophageal manometry. This isn’t a scan or an X-ray. It’s a pressure test. A thin, flexible tube with sensors is inserted through the nose and into the esophagus. As you swallow sips of water, the sensors measure the strength, timing, and coordination of each muscle contraction.For decades, this was done with a single pressure sensor. Today, most hospitals use high-resolution manometry (HRM). It has 36 sensors spaced just 1 cm apart. That means doctors can see exactly where and how the esophagus is failing. The data creates a color-coded map-like a weather map showing pressure storms across the esophagus. This is how conditions like achalasia, nutcracker esophagus, and jackhammer esophagus are identified.
The Chicago Classification: A New Standard
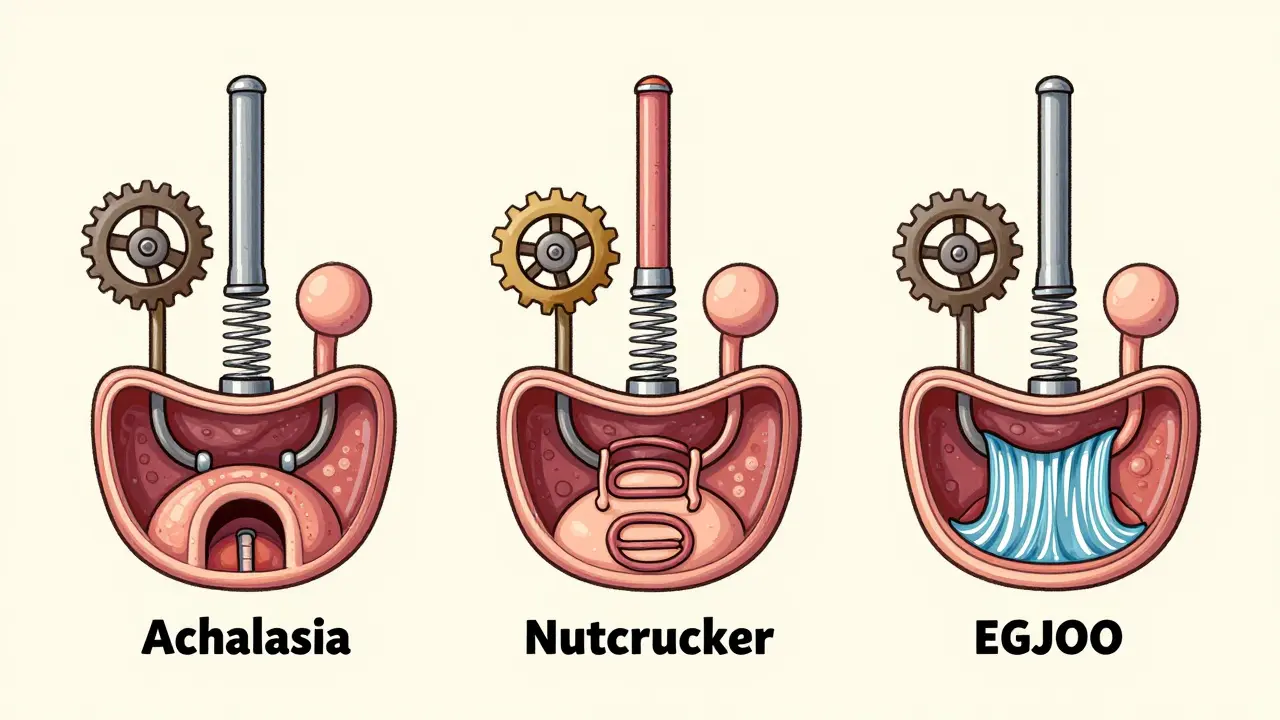
In 2023, the latest version of the Chicago Classification (v4.0) became the global standard for diagnosing these disorders. Before this, doctors often disagreed on what counted as "abnormal." Now, every major medical center uses the same criteria. For example:- Achalasia: The lower esophageal sphincter (LES) won’t relax. Peristalsis is absent or chaotic. It’s split into three types: Type I (no contractions), Type II (pan-esophageal pressurization), and Type III (spasms).
- Nutcracker esophagus: Contractions are strong-over 180 mmHg-but coordinated. Often causes chest pain.
- Jackhammer esophagus: Even stronger contractions, with a distal contractile integral over 5,000 mmHg•s•cm. This can feel like a heart attack.
- Esophagogastric junction outflow obstruction (EGJOO): The LES pressure is high, but peristalsis is normal. This is a newer category introduced in 2023.
These distinctions matter. Treatment changes based on the type. Mislabeling one as another can lead to ineffective or even harmful care.

Manometry vs. Other Tests
Barium swallow tests used to be common. You drink chalky liquid, and X-rays track its movement. But they miss up to 22% of motility disorders. HRM catches 96% of achalasia cases-far better than barium’s 78%. Another option, EndoFLIP, measures how stretchy the esophagus is. It’s useful for evaluating obstruction, especially in complex cases.But manometry isn’t perfect. The tube can be uncomfortable. About 35% of patients report moderate to severe discomfort. And it’s not available everywhere. Only 95% of academic hospitals in the U.S. have HRM. In rural areas or low-income countries, access is rare. That’s why some patients wait years for a diagnosis. One survey found 68% waited 2-5 years and saw at least three doctors before getting the right answer.
Treatment: One Size Doesn’t Fit All
Treatment depends entirely on the diagnosis.- Achalasia: The gold standard is surgery-laparoscopic Heller myotomy (LHM), where the tight LES muscle is cut. Success rates are 85-90% at five years. A newer option is POEM (peroral endoscopic myotomy), done entirely through the mouth. It’s equally effective but carries a higher risk of reflux-44% of patients develop esophagitis within two years.
- Pneumatic dilation: A balloon is inflated in the LES to stretch it. It works for 70-80% of patients initially, but 25-35% need repeat procedures within five years.
- Nutcracker and jackhammer: These are harder to treat. Calcium channel blockers or nitrates can help relax the muscle. Botox injections into the LES are sometimes used. In severe cases, surgery may be considered.
- Secondary disorders: If the cause is scleroderma, treatment focuses on the underlying disease. The esophagus may need dietary changes, medications, or even feeding tubes in advanced cases.
There are also emerging options. The LINX device, a magnetic ring implanted around the LES, is now being tested for select achalasia patients with preserved peristalsis. Early results show 75% symptom improvement at one year. And wireless capsules like the SmartPill let patients wear a tiny sensor for 24-48 hours, recording motility while they go about their day. It’s less invasive and correlates with HRM at 85% accuracy.
What Patients Say
Real stories highlight the gap between diagnosis and relief. One Reddit user wrote: "After my POEM, I ate a burger for the first time in seven years. I cried." Another shared on a health forum: "I was on PPIs for eight years. My doctor said I had GERD. Manometry revealed jackhammer esophagus. Everything changed after that."But not all experiences are positive. Some patients get labeled with "minor motility disorders"-abnormal patterns that may not even cause symptoms. Experts warn against overtreating these. As Dr. C. Prakash Gyawali put it: "We can’t treat every weird pressure wave. Many are just noise."
Why This Matters Now
The market for esophageal diagnostic tools is growing fast-projected to hit $410 million by 2028. More hospitals are investing in HRM. Fellowship programs now require motility training. AI tools are being trained to read manometry tracings with 92% accuracy, outperforming untrained humans. But access remains unequal. If you live outside a major city, getting tested might mean traveling hundreds of miles.The key takeaway? If you have persistent dysphagia, especially if PPIs don’t help, don’t accept "it’s just acid reflux." Ask for manometry. It’s the only test that shows how your esophagus actually moves. And with the Chicago Classification v4.0, doctors now have a clear roadmap to diagnose-and treat-these disorders accurately.
Can dysphagia be caused by something other than motility disorders?
Yes. Dysphagia can also stem from structural issues like esophageal strictures, tumors, or external compression from enlarged lymph nodes or thyroid glands. That’s why doctors start with an endoscopy-to rule out these problems before testing motility. If the esophagus looks normal, then motility disorders become the next focus.
Is high-resolution manometry painful?
It’s uncomfortable, but not usually painful. The tube is thin and lubricated. Most people feel pressure or a gag reflex when it’s inserted. Numbing spray helps. About 35% of patients report moderate discomfort, but only 5% say it’s unbearable. Breathing slowly and staying relaxed helps. The whole test takes about 20-30 minutes.
Can I have an esophageal motility disorder without having symptoms?
Rarely, but yes. Some people have abnormal manometry results with no swallowing problems. These are called "minor motility disorders" under the Chicago Classification v4.0. Experts now advise against treating these unless symptoms develop. Treating them unnecessarily can lead to complications from surgery or medications that aren’t needed.
How long does it take to get results from manometry?
The test itself takes less than an hour. But interpreting the data takes time. A trained specialist needs to analyze the pressure patterns, which can take several hours. Most clinics deliver results within 3-7 business days. If the case is complex or requires a second opinion, it may take longer.
Are there non-surgical treatments for achalasia?
Yes. Pneumatic dilation and botulinum toxin (Botox) injections are non-surgical options. Dilation stretches the LES and works well for many patients, though it may need repeating. Botox temporarily paralyzes the muscle, giving relief for 6-12 months. These are often used for older patients or those who can’t undergo surgery. But they’re not permanent fixes-surgery remains the most durable solution.

Steve DESTIVELLE
February 12, 2026 AT 15:19So we’re just supposed to accept that the esophagus is this mysterious muscular goddamn labyrinth that no one fully understands until it stops working and you’re left choking on your own dinner like some kind of tragic Shakespearean fool
Peristalsis isn’t just biology it’s poetry and when it breaks you don’t get a warning you get silence
The Chicago Classification v4.0? It’s not a diagnostic tool it’s a language we finally learned to speak after decades of screaming into the void
And yet we still treat symptoms like they’re the disease
PPIs for everything because it’s easier than admitting we don’t have the right tools or the patience to use them
Manometry isn’t uncomfortable it’s an act of rebellion against ignorance
Every pressure wave measured is a silent scream from a body that wasn’t heard
We label people with "minor motility disorders" like they’re glitches in a system that’s supposed to be flawless
But the body doesn’t glitch it communicates
And if we’re too lazy to listen we’re not just misdiagnosing we’re erasing
There’s no algorithm that can replace the quiet courage of someone who keeps going back to doctors until they’re finally believed
It’s not about technology
It’s about dignity
And dignity doesn’t come from a color-coded map
It comes from being seen
Alyssa Williams
February 14, 2026 AT 13:20This is so important. I had dysphagia for 5 years and was told it was GERD. I was on PPIs nonstop. Then one doctor finally ordered manometry. Jackhammer esophagus. Changed everything. No more PPIs. No more fear. Just food. Just life.
Stephon Devereux
February 15, 2026 AT 18:32Alyssa’s story is why we need to stop treating symptoms and start treating systems
The esophagus isn’t broken because it’s weak
It’s broken because we stopped listening to how it works
High-resolution manometry isn’t just a test
It’s a conversation
And the Chicago Classification? It’s the dictionary we needed to understand what the body was trying to say all along
POEM isn’t just a procedure
It’s a revolution
One that lets people eat burgers again without fear
And that’s not medicine
That’s magic
But magic only works if you believe in the process
So if you’re reading this and you’ve been told "it’s just acid" - push back
Ask for the test
Because your body isn’t exaggerating
It’s screaming
steve sunio
February 16, 2026 AT 00:04Neha Motiwala
February 17, 2026 AT 19:15They’re hiding something. Why is this only available in big cities? Why is it so expensive? Who profits from people suffering for years? Big Pharma? The hospitals? The equipment makers? The system is designed to keep people confused and dependent
And don’t even get me started on the Chicago Classification - it sounds like a corporate branding scheme to me. Who even wrote this? Are they getting paid by the companies that make the manometry tubes?
My cousin had this and they told her she had "minor motility" - then she lost her job because she couldn’t eat. No one helped. Now she’s on a feeding tube. And the doctors? They just shrugged.
There’s a cover-up here. You feel it too, don’t you?
Jack Havard
February 19, 2026 AT 18:43Interesting. But let’s be real - how many of these "disorders" are just normal variations that got overmedicalized?
Manometry picks up weird patterns because it’s sensitive as hell
But correlation isn’t causation
My uncle had a "nutcracker" result and zero symptoms. They gave him meds. He got dizzy. He quit. He’s fine now
Maybe we’re turning healthy quirks into diseases because we need to sell tests
And what about those "minor" classifications? Sounds like a way to monetize anxiety
I’m not saying it’s all nonsense
But we’re definitely overtreating
And I’m tired of being told to trust the system when the system has no idea what it’s doing
Rob Turner
February 21, 2026 AT 09:46I'm from the UK and we've got the same problem - HRM is only in a handful of hospitals
My sister waited 3 years. She flew to London for the test. Cost her £1200 out of pocket
And then they told her she had EGJOO - a diagnosis that barely existed 5 years ago
It’s wild how fast this field is evolving
But the infrastructure? Still stuck in the 90s
POEM and LINX? Amazing
But if you live in Wales or Northern Ireland? Good luck
We need a national rollout. Not just for the rich
Or the well-connected
Or the ones who can scream loud enough
Gabriella Adams
February 21, 2026 AT 14:30Just wanted to say - thank you for writing this. As a GI nurse, I’ve seen patients cry because they finally got answers after 7 years
And I’ve seen others dismissed because their endoscopy looked "normal"
Manometry changed everything
It’s not flashy
It’s not glamorous
But it’s the most honest test we have
It doesn’t lie
It doesn’t guess
It just measures
And sometimes - that’s all we need
To stop treating the symptom
And start treating the system
Vamsi Krishna
February 22, 2026 AT 12:35Let me tell you something
I had jackhammer esophagus
It felt like my chest was being crushed by a thousand fists
I thought I was having heart attacks
My wife called 911 twice
Doctors said stress
Then acid
Then anxiety
Then I found a manometry specialist in Delhi
He looked at the tracings
And said - "This isn’t normal. This is fire"
He gave me nifedipine
And told me to eat slowly
And breathe
And now I can eat rice without fear
But I still wake up some nights
And touch my chest
Just to make sure it’s still there
Don’t let anyone tell you it’s "just a weird pressure wave"
It’s your body screaming
And if you don’t listen
You’ll forget how to swallow
Craig Staszak
February 23, 2026 AT 22:39Really appreciate this breakdown. I’ve been following motility research since my dad had achalasia. POEM was a game-changer for him - no incisions, went home the next day. But yeah, access is insane. We drove 400 miles. Took two weeks off work. And the cost? Insurance barely covered it.
What we need isn’t more tech - it’s more equity. A world where a kid in rural India or rural Alabama has the same shot at a diagnosis as someone in Boston or London.
That’s the real revolution.