Asthma: How to Spot It, Manage Flare-ups, and Breathe Easier
Worried every cough might be the start of an asthma attack? Asthma often shows up as wheeze, shortness of breath, chest tightness, or a cough that gets worse at night or with exercise. Knowing early signs and having a plan cuts panic and keeps you out of the ER.
Start with a clear plan. Ask your doctor for a written asthma action plan that says which medicines to take daily, how to treat symptoms, and when to seek help. Keep it where family or roommates can see it so everyone knows what to do if breathing gets worse.
Make inhalers and meds actually work
Inhaler technique matters more than most people think. Use a spacer if you have a metered-dose inhaler — it helps medicine reach your lungs instead of landing in your mouth. A quick checklist: shake the inhaler, breathe out fully, press once while breathing in slowly, hold your breath 5–10 seconds, then breathe out. If you cough or taste medicine in your mouth, you might be doing it wrong.
Know the types of meds without getting lost in jargon. Quick-relief inhalers (short-acting bronchodilators) stop attacks fast. Controller medicines, like inhaled corticosteroids, reduce inflammation over time and lower the chance of attacks. Don’t stop controllers because you feel better — that’s often when problems come back.
Cut triggers out of your daily life
Triggers vary, but common ones are tobacco smoke, pet dander, dust mites, mold, strong odors, cold air, viral infections, and exercise. Small changes add up: use allergen-proof mattress covers, wash bedding weekly in hot water, keep humidity under 50%, and avoid smoke. If exercise triggers symptoms, use your quick-relief inhaler 10–15 minutes before activity, as your doctor advises.
Track symptoms so you see patterns. A simple symptom diary or a peak flow meter can show when control is slipping. Peak flow readings are grouped into three zones: green means good control, yellow warns of worsening, and red means seek urgent care. Your doctor will set the numbers for you.
Know when to get emergency help. Call 911 or go to the ER if you can’t speak full sentences, lips or face turn blue, you’re using neck and chest muscles to breathe, or quick-relief meds don’t help after a few minutes. Don’t wait until symptoms become severe.
Small lifestyle steps help a lot: maintain a healthy weight, get flu and COVID vaccines each year, avoid indoor pollutants, and manage allergies. Work with your healthcare provider to review your meds at least once a year or sooner if symptoms change.
Want help putting a plan together? Bring this list to your next appointment and ask for an action plan and an inhaler check. Having clear steps and the right technique gives you the best chance to stay breathing easy.
The Link Between Obstructive Pulmonary Disease and Asthma
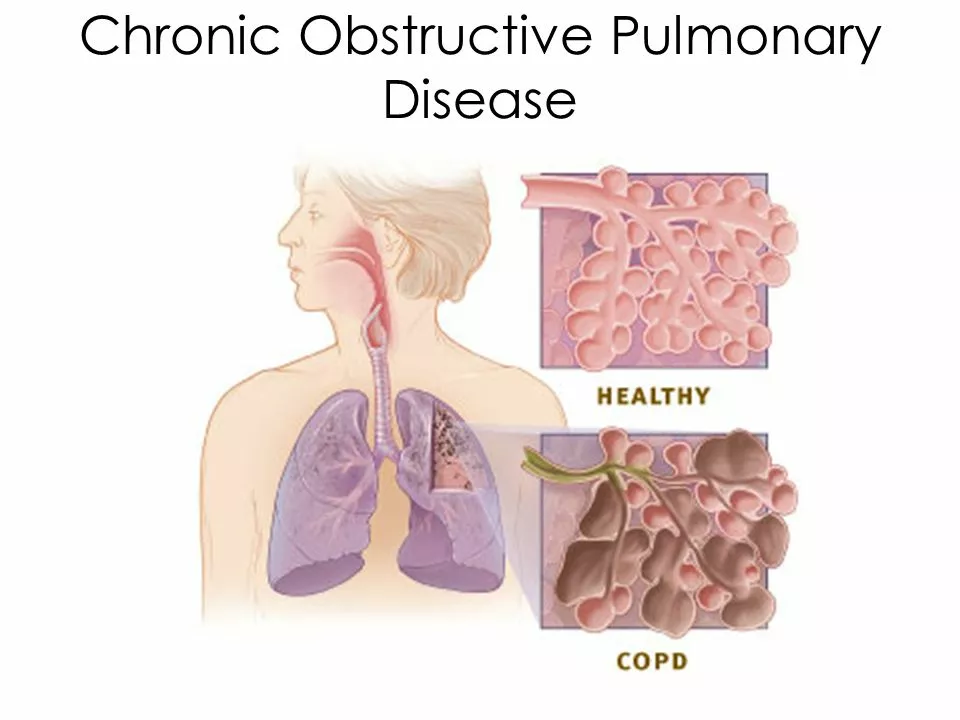
In a recent blog post, I came across some fascinating information about the connection between obstructive pulmonary disease (COPD) and asthma. Both are chronic respiratory conditions that cause breathing difficulties, but they have different causes and treatments. It turns out that some people may have both conditions, which is known as asthma-COPD overlap (ACO), making it challenging to manage and treat their symptoms. Studies have shown that people with ACO experience more frequent exacerbations and a more rapid decline in lung function compared to those with asthma or COPD alone. It's essential to be aware of this link and get a proper diagnosis to ensure the most effective treatment plan for your condition.
- May 20 2023
- Tony Newman
- 20 Comments
